Bunions (Hallux Valgus)
Bunions are quite common, and occur when the big toe pushes towards the adjacent toes, making the joint at the base of the big toe protrude outwards. This joint is the metatarsal to the phalanges (the equivalent joint in the hand is the base of the thumb, which is where the bunion would be, the next part of the thumb is the proximal phalanx and lastly the distal phalanx - being the bone at the end of the thumb).
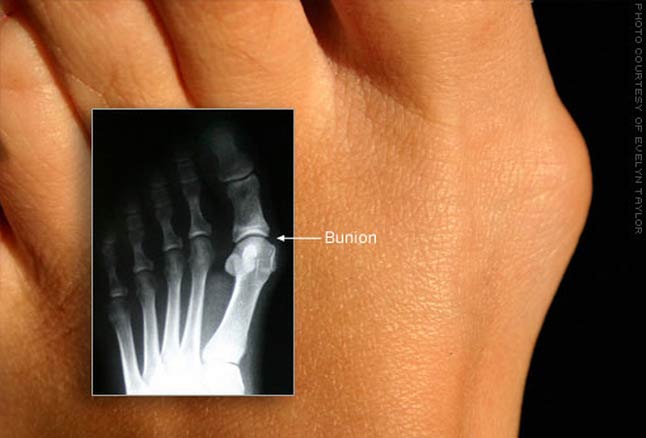
Patients often complain that the skin in the affected area may chafe when wearing shoes, causing pain. This can result in limited mobility owing to pain – if the patient cannot find suitable footwear.
Treatment
A conservative treatment could be to wear adaptive shoes, eg. using inner soles of soft protective material to relieve rubbing against the inner aspect of their shoes.
Surgical options include removing the bone (osteotomy). There are a number of different types of operations that can be performed but generally speaking the procedure is undertaken with an incision made over the bunion (under either local or general anaesthetic).
The metatarsal bone is broken and re-fixed, using plates, screws or ‘K-wires’, which are temporary wires that can be pulled out when the bones have united. At operation the wound is closed and covered, and the foot may be held fixed by plaster or equivalent so that the broken bone can heal in the right position.
Complications
The frequency of a bunion recurring is between 1-2% post-operatively, with increased pain being experienced in 1%, the majority having reduced pain or no pain.
Reports of experiences state that about 86% of patients were very pleased or pleased, with 4% regretting having had the operation and 4% being dissatisfied.
Other complications included osteomyelitis (infection of the bone), necrosis of the bone (death of the bone), and delay or failure of union of the bone (i.e. the broken bone does not heal) in up to 1% of cases.
In the NICE guidance on this topic, specialist advisers listed the following complications:
- ‘Nerve injury including complex regional pain syndrome
- Toe stiffness
- Skin necrosis
- Osteomyelitis
- Deep vein thrombosis
- Tendon injury
- Removal of fixation screw
- Recurrent deformity
- Fracture
- Tender scars
- Skin sensitivity
- Theoretical adverse events could include burning soft tissue, damage to foot blood vessels, an inflammatory reaction to bone debris, and first metatarsal malpositioning, shortening or necrosis.’
Another problem that can occur later on is a change in how the biomechanics of the foot functions, so that the weight on the foot is altered which can lead to stress fractures, a change in the gait and even different pressures put onto the knees, hips and spine.
Adjacent toes can also be affected e.g. arthritis, hammer toes and other tissues in the leg, such as the Achilles tendon on the affected side.
MEDICOLEGAL ASPECTS
NICE guidance on the use of minimally invasive techniques is clear that the safety profile of this technique requires that the surgeon/team undertaking the procedure MUST:
- Ensure that patients and their carers understand the uncertainty about the procedure’s safety and efficacy and provide them with clear written information. In addition, the use of NICE’s information for patients (‘Understanding NICE Guidance’) is recommended
- Audit and review clinical outcomes of all patients having surgical correction of bunions using minimal access techniques
- Inform the clinical governance leads in their Trusts
If you want further information about this particular topic, or wish to discuss the possibility of bringing a claim for Clinical Negligence - or indeed any other type of injury, please contact the Dutton Gregory Clinical Negligence Team on (01202) 315005, or email contact@duttongregory.co.uk
NB This article does not constitute legal advice and should not be relied on as such. No responsibility for the accuracy and/or correctness of the information and commentary set out in the article, or for any consequences of relying on it, is assumed or accepted by any member of Dutton Gregory LLP.






